Having just started to come out of a bad incidence of PEM I realised it’s something I’ve not specifically posted about. Yet it’s been a huge part of my life for over three years. So I’m going to try to explain in personal terms just how incredibly debilitating it is. A little background is probably necessary.
According to the NIH* “Post-Exertional Malaise (PEM) is a cardinal symptom of the illnesses referred to as Myalgic Encephalomyelitis (ME), Myalgic Encephalomyelitis/chronic fatigue syndrome (ME/CFS), and chronic fatigue syndrome (CFS).”
A cardinal symptom is one that must be experienced by the patient to confirm diagnosis of the condition, in this case ME. Although my official diagnosis of ME wasn’t confirmed until about eighteen months ago, my GP and I are both in agreement that this has been ongoing for me since the time of my original RA diagnosis.
So, what exactly is it? And how does it differ from the fatigue experienced by patients with RA or other autoimmune conditions?
The NIH* states that “Unlike generalized fatigue, PEM is much more profound and reduces daily functioning. This symptom is characterized by a delay in the recovery of muscle strength after exertion, so it can cause patients to be bedridden for multiple consecutive days.”
And this is exactly what I’ve just been through. More recent studies into PEM recognise that the earlier criteria of ‘exercise’ was misleading and led to confusion amongst patients affecting diagnosis, ‘exertion’ is now used to provide a clearer picture, and it’s recognised that this can be mental or physical exertion, and that the physical exertion has a much lower baseline than in the standard population, as patients with ME are rarely able to exercise.
So we know PEM is profound and reduces daily functioning. But what does that look like? And how does it feel in real patient terms?
The NIH* describes it as “a worsening of ME/CFS, ME and CFS symptoms including fatigue, headaches, muscle aches, cognitive deficits, insomnia, and swollen lymph nodes. It can occur after even the simplest everyday tasks, such as walking, showering, or having a conversation.”
Seriously? Showering? Having a conversation? Actually yes, and in my experience having conversations, chatting, talking, call it what you will is incredibly draining. That doesn’t mean it can’t be enjoyed, but it does mean I’ll often pay for it later.
I’ll try and describe as clearly as I can how I was affected this weekend. I came home Sunday evening from visiting my Dad, which involves more driving than I would usually do. I want to make it clear here that I’m not blaming you Dad!! ❤️ Going to Waitrose or even popping out for lunch can have exactly the same effect. That’s the point. It doesn’t take much. And it doesn’t have to be physical. Dealing with simple paperwork for a short time can do the same thing.
So, Sunday afternoon. The first sign for me is usually yawning. Before I had ME I never thought of yawning as being a physical thing, but this can drop me to my knees. It’s like my whole body yawns with me. A couple of friends in my regular social circle will spot this a mile off now, and they’ll simply say ‘time to go home’. Apparently I suddenly look exhausted. Always attractive!
I’d say that on average within twenty minutes of this yawning starting I’ll be asleep, there is no choice, no putting it off. It’s like my whole body is simply shutting down. My head stops thinking, my muscles go heavy, and I can barely walk.
I lay down on the sofa at about six pm on Sunday, and only came to properly at about 6am this morning. So that’s 36 hours of basically being unconscious. I know I woke twice when my alarms went off to take my meds, and I know there was a third alarm I ignored so I missed a dose. I know I briefly came to and made a coffee at about 7pm on Monday, and it took everything I had to get into the kitchen and back. The rest is a blur of weird dreams involving a pub fire, going swimming in Italy and a trip to a theatre. Strange but true.
So that’s 36 hours lost so far. When I woke at 6am this morning I knew the worst had passed, the almost coma like feeling had gone, and my mind is awake to some small extent. Enough to slowly write this at least. But I have zero energy, and little concentration. From experience it will take another 24 hours at least before I’m able to actually get up and shower. I won’t be able to read or follow a TV plot properly, and I will probably sleep a lot today, though hopefully more refreshing sleep, not the passed out exhausted-ness of the past two days. Although it’s not an experience I’ve had I imagine I probably feel about the same as a marathon runner the day after, when everything hurts and you can barely move!
This is not a rare occurrence, it happens about once a week. I can lose from one to three days. I do pace my activities quite carefully, plan down days around days I have to be up and out, whether for medical appointments or social. I live alone so I try to get out three times a week for a couple of hours each time, usually a couple of coffees or soft drinks with friends. It’s incredibly easy to become isolated with chronic illness and it’s so very important we don’t.
So today will be a ‘sofa day’, as it happens it’s very rainy and dark outside so a perfect day for a couple of daft movies and snoozing. Then, fingers metaphorically crossed, I’ll feel human again tomorrow 😊
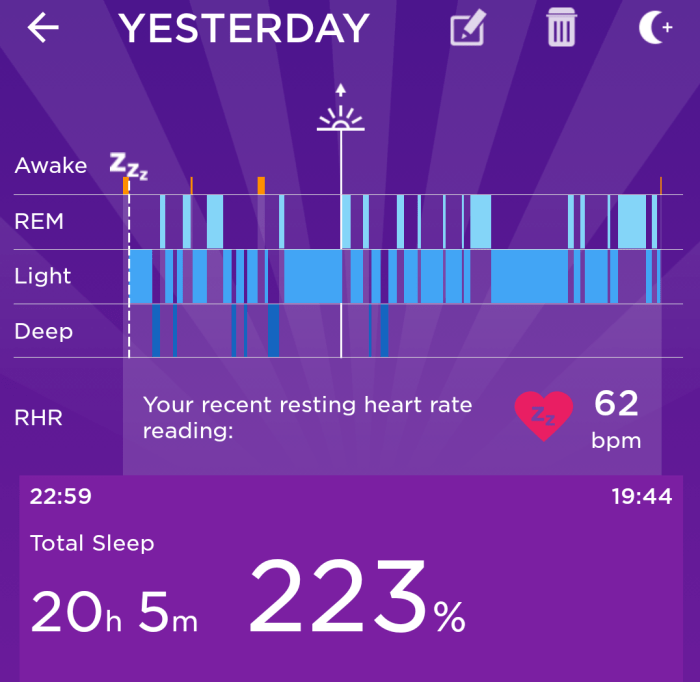
Footnote – it’s curious but common in #chroniclife to feel the need to validate ones symptoms and experiences, especially with something like ME which is incredibly still dismissed by some doctors. In this instance I’m actually glad I was wearing my sleep tracker, which has recorded 23 hours of sleep for yesterday. Proof!

*I have referred to and quoted from the American NIH or National Institute of Health because I find their website carries clear and up to to date articles. The full text that I’ve quoted from can be found here.