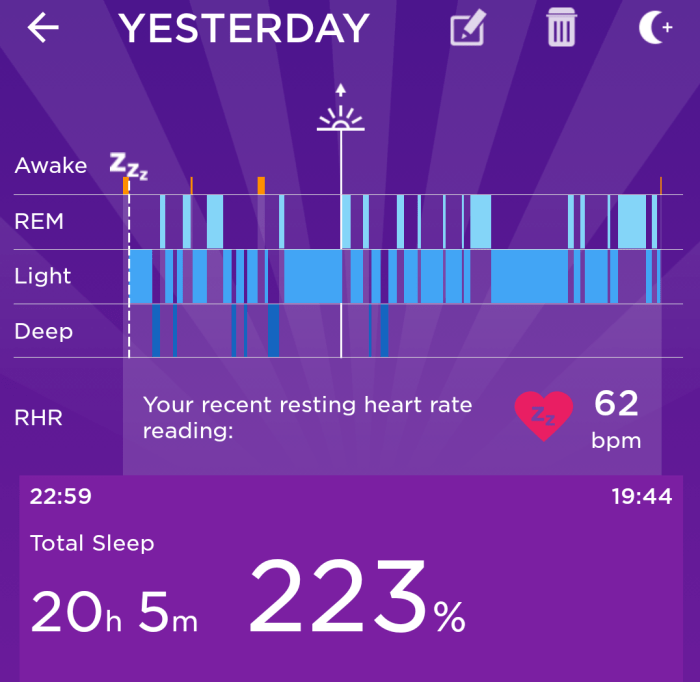
Some of you will be aware I write when I need to process. Never more necessary than this week.
I’m struggling right now, both physically & mentally. This is totally down to our disastrous current government. I make no apologies for being political when those very politics are affecting my physical & mental health.
I received notification in June/July this year that even though I had been previously awarded lifetime DLA (Disability Living Allowance) for my chronic & progressive conditions, due to govt changes to the benefit system – namely the introduction of the new PIP (Personal Independence Payment) benefit – I had to reapply. Yes, reapply.
You’d have thought the sensible thing to do for people with lifetime disability awards would be a simple transfer, but no. Reapply as if you’re a completely new claimant. There was an option to allow them to access your previous assessment records for DLA to support your claim – “if they are still available”. Yes, it appears the DWP may have failed to actually keep records properly. Who’d have guessed.
I want to be clear here before moving onto the effect this process is having on me personally – the only reason the govt have rolled out PIP is to get disabled people off benefits. It’s that simple & that barbaric. A UN report in 2017 “accused the Tories of creating a ‘human catastrophe’ in the UK” which violates disabled people’s human rights, the text below is quoted from The Canary, the full article is available here

The UN are currently carrying out another investigation into UK poverty and the impact the current government has had on this, looking at key areas including these listed below – text again is from The Canary, full article is available here.

I kind of wanted to be clear on this – this is not me as a benefit claimant just being awkward or heaven forbid “ungrateful” – but a widely acknowledged truth. Disabled people are being disadvantaged by this government, the facts prove that. The United Nations knows it.
So, back to to this process. I had to call to apply after receiving the letter which was incredibly difficult for me – anything to do with benefit changes causes me severe anxiety – I was physically shaking when I rang, despite being prepared by Citizens Advice on what to expect so I had the information I needed right in front of me. It took a stomach churning twenty minutes. Just to ask for the form.
Once the form arrives in the post there is a four week deadline for completion. The earliest appointment Citizens Advice had was for almost six weeks away. So again I had to go through the ordeal of phoning, this time to request an extension which thankfully was granted.
I cannot begin to describe the vile process of completing that form, even with a trained & sympathetic advisor. I can’t write for any length of time myself because of the RA in my hands, so they had to complete the form for me. It’s invasive, incredibly personal & embarrassing. Answering questions on what medications you take, their side effects, how often you manage to wash yourself, use the toilet, leave the house, eat, get out of bed, the assistance you need but don’t get, and the intimate details of every symptom of your conditions & disability from bowel movements to insomnia, light sensitivity to Myoclonic Jerks.
The awful thing is on a daily basis you are mostly able to avoid thinking about the vastness & sheer weight of multiple conditions & symptoms alongside chronic unceasing pain, you simply deal hour by hour because that is manageable, mostly. This is like plunging into the abyss with your eyes taped wide open. It’s not an exaggeration to say it’s traumatic.
Every tiny personal detail of your life is discussed & transcribed, ready to be pored over by faceless strangers – without the requisite medical knowledge – but with the power to remove your income & your car & leave you destitute & housebound. Yes, it’s that f*cking huge.
So – my appointment with the lovely & very empathetic lady at Citizens Advice? Three hours. Three grueling & exhausting hours. And I wasn’t done yet.
It took me another two hours at home to go through, copy & annotate twenty-seven separate pieces of medical evidence going back about 18 months. Scan reports, surgical reports, consultants letters, radiography reports, it all went in there. This took me about three days.
So finally it all went into the post. I had a text on the the 8th August to say my form had been received.
I then heard nothing until Saturday 3rd November when a letter dropped through my door. Yes, just over twelve weeks, or 3 months. Every single day since August my anxiety has grown worse. My depression is also pressing at the edges of my consciousness, whispering of hardships & darkness. My GP is fully aware & we’re monitoring my mental health, the frustration is that we know the exact cause & have no power to remove it.
So the last couple of days I’ve basically gone turtle. I’ve retreated inside my shell, alternating between Netflix & reading depending on my ability to concentrate. The minute I stop either my thoughts are immediately back to this planned assessment. I feel dreadful as stress flares everything. Fortunately I have a wonderful friend who has agreed to be with me for the appointment which is incredibly helpful.
My next task which I couldn’t bring myself to do today is to call them & ask why they’ve not taken on board the request on the form from Citizens Advice & myself for a home visit, and see if its possible to change it. Honestly from what I’ve heard I’m not particularly hopeful.
Then I need to prepare, think of this as a job interview but twenty times worse. Its so easy with fatigue, anxiety & brain fog for me to use the wrong words, forget whole symptoms & conflate conditions. It’s basically a quiz about me where I can get the answers wrong much too easily. I’m terrified of this, and not without reason – so many horror stories of poor assessments are a matter of record.
One last note – DWP or whomever, if you’re reading this and thinking even for one second “well if she can write a blog that makes sense she can work” you are stunningly misinformed about what being chronically ill & disabled looks like.
This, as with many of my posts takes hours – but never all at once. Initial thoughts, a few notes, finding links, remembering what the hell I was talking about when I lose thread mid sentence, stopping for sleep or rest, editing, rechecking, a final read through to make sure I haven’t made a compete idiot of myself. It all takes precious time and energy spread out over days, to do something that when I was well I could have rattled off in ten minutes.
This is my reality, please simply believe me.
PS – for anyone who has bought into MSM (Main Stream Media)’s outright fairy tales about benefit fraud & demonisation of claimants – here’s the real deal from the government’s own data. A tiny 1.2% of benefit claims are fraudulent.
“Like HMRC, the DWP also estimates fraud and error for its benefit payments. Its most recent estimate shows that overpayments to claimants in 2017/18 were £3.8bn, or 2.1% of its total bill. Of this, 1.2% (£2.1bn) of its £177.5bn budget was claimant fraud. Full article here.